Blog
Digestive Cancer Screening
23 Jun 2022
What is screening?
Screening is looking for cancer before a person has any symptoms. The aim is to detect cancer at an early stage. When cancers are detected an an earlier stage, the likelihood of cure or prolonging life is higher. By the time symptoms appear, cancers have usually spread and treatment is more challenging and cure rates lower.
A screening test is recommended based on defining a population of people who are at risk, secondly proving that a screening test is beneficial in improving patient outcomes and lastly the screening interval so that the test is economically viable if this screening test is aimed at the entire population. It is important to note that screening tests are performed in people without symptoms.
If a screening test result is abnormal, you may need to have more tests done to find out if you have cancer. These are called diagnostic tests.
- Colon Cancer Screening
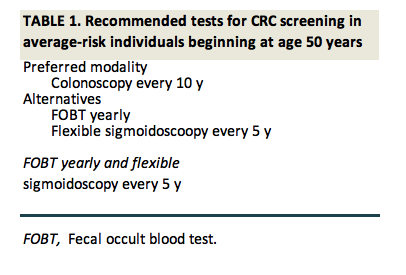
Colon cancer is the most common cancer in men and the second most common cancer in women in Singapore. The incidence for colon cancer has risen dramatically over the last 30 yrs and risk factors include male gender, race (chinese being at highest risk in Singapore), family history, older age, diabetes mellitus and obesity.

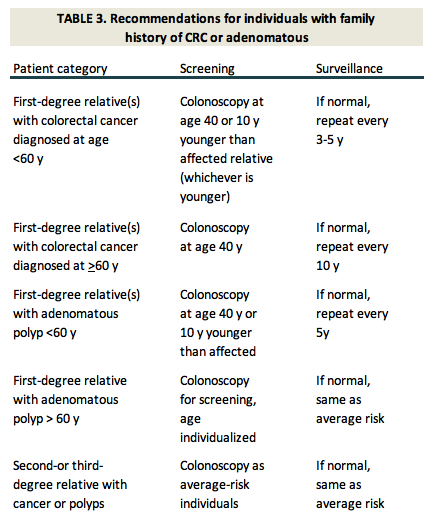
FAP – Familial Polyposis Coli
HNPCC – Hereditary Non-Polyposis Colon Cancer

- Liver Cancer Screening
Screening for liver cancer is recommended in patients who are hepatitis B carriers or that have evidence of advanced fibrosis or cirrhosis. Liver fibrosis and cirrhosis should be assessed in all patients with underlying liver disease either using non-invasive modalities such as Fibroscan liver stiffness measurement or liver biopsy. Ultrasound is the screening modality of choice for liver cancer because of its cost-effectiveness and patient acceptability. The screening interval should be either 6 monthly or annually.
- Stomach (Gastric) Cancer Screening
- Gastric cancer is one of the most common cancers worldwide. However, there are significant differences in the incidence of gastric cancer by region and hence universal gastric cancer screening may not be cost-effective on a population wide scale.
- Studies suggest that endoscopic screening is more sensitive than radiographic screening for gastric cancer.
- Although screening for gastric cancer may be cost-effective in high-risk subgroups, whether screening improves clinical outcomes (ie, gastric cancer-related mortality) is unclear. While some observational studies suggest that screening contributes to detection of early gastric cancer and an overall decline in gastric cancer mortality, we await data from large controlled trials.
- Recommendations for screening differ based on the region or country based on the endemic incidence of gastric cancer. Universal or population-based screening for gastric cancer has been implemented in some countries with a high incidence of gastric cancer (eg, Japan, Korea, Venezuela, and Chile). In areas of low gastric cancer incidence, screening for gastric cancer with upper endoscopy should be reserved for specific high-risk subgroups. Individuals at increased risk for gastric cancer include those with gastric adenomas, pernicious anemia, gastric intestinal metaplasia, familial adenomatous polyposis, and Lynch syndrome.
- Oesophageal Cancer Screening
Oesophageal cancer is a disease in which malignant (cancer) cells form in the tissues of the oesophagus. Oesophageal cancer is found more often in men. Other risk factors include smoking, heavy alcohol use, and Barrett esophagus. Currently there are no recommendations for universal oesophageal cancer screening for the general population. However patients with Barrett’s oesophagus should undergo interval surveillance for oesophageal cancer.
- Pancreatic Cancer Screening
There is currently no recommendation for universal screening in the general population for pancreatic cancer using either abdominal palpation, ultrasonography, or serologic markers. However, diagnostic contrast imaging or endoscopic ultrasound may be useful in diagnosing pancreatic cancer in asymptomatic individuals with elevated cancer markers or in diagnosing mass lesions detected on health screening.
We’re Here To Help. Get In Touch.
Connect with GUTCARE: Your Path to Digestive Health and Wellbeing. Contact us for specialised care and professional consultation. Your journey to optimal digestive well-being begins here.







