What Is 24Hr Ph
Impedance Test?
What is Endoscopic Retrograde Cholangiopancreatography (ERCP)?
ERCP is an advanced endoscopic technique which combines interventional endoscopy and interventional radiology to treat conditions in the bile ducts and the pancreatic duct. These ducts are drainage channels to drain bile and pancreatic juice from the liver and the pancreas respectively. Special techniques are required to enter these ducts. Thereafter, various instruments are passed into the ducts to perform various diagnostic and therapeutic interventions. ERCP is a safer and less invasive approach to treat conditions in these areas instead of complex major surgery. ERCP has become the international standard of care in many of these conditions.
PROCEDURE
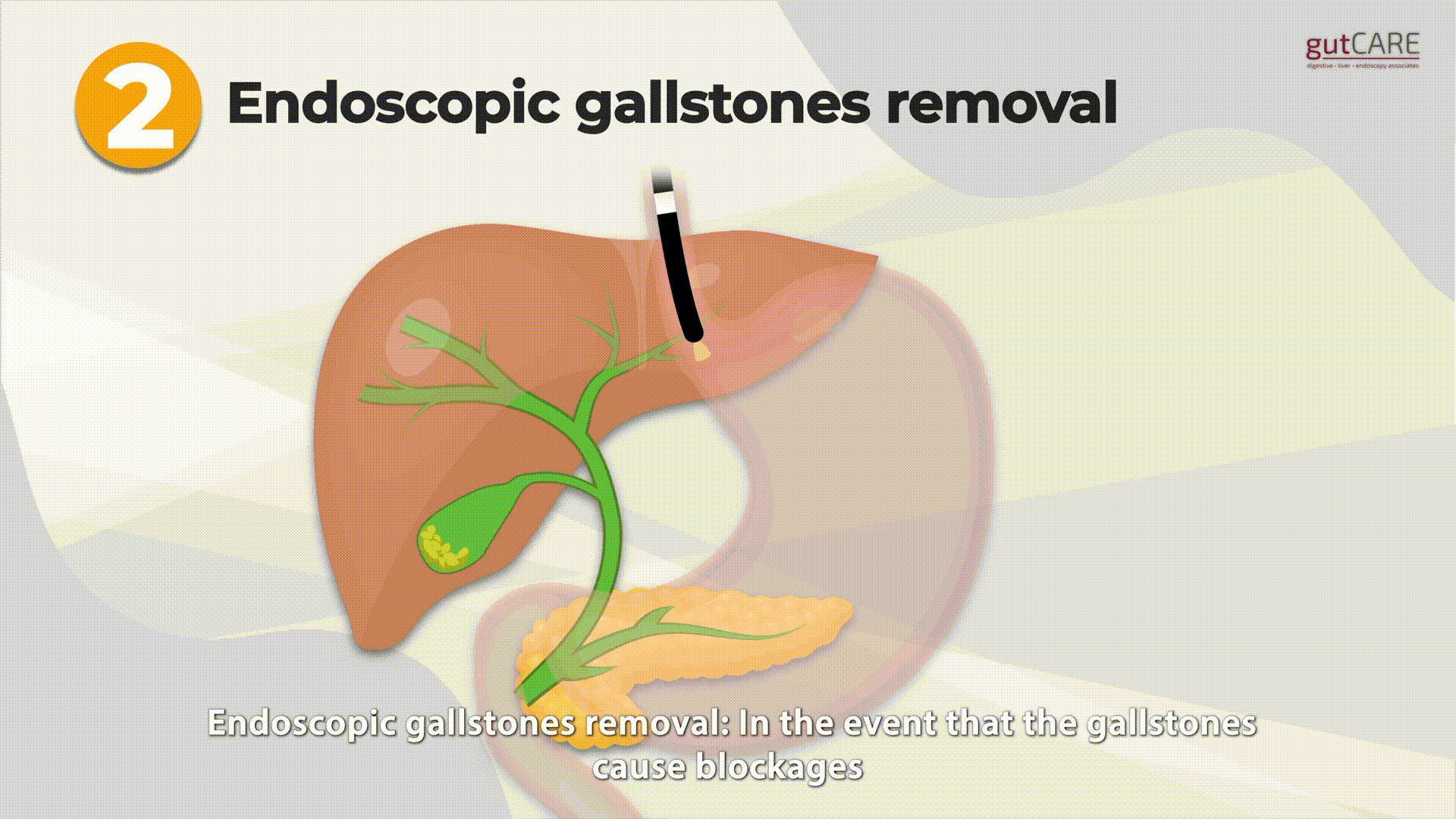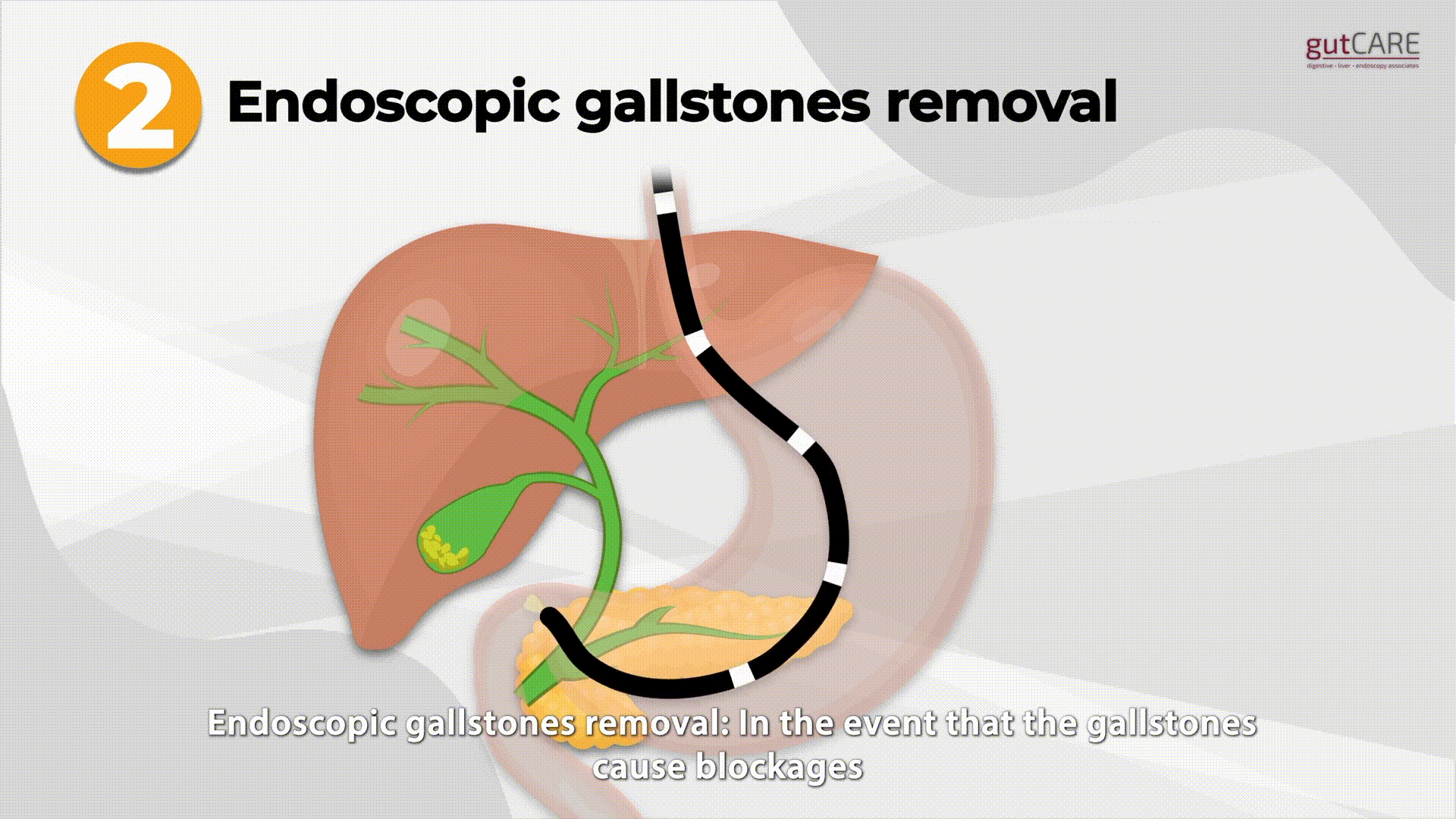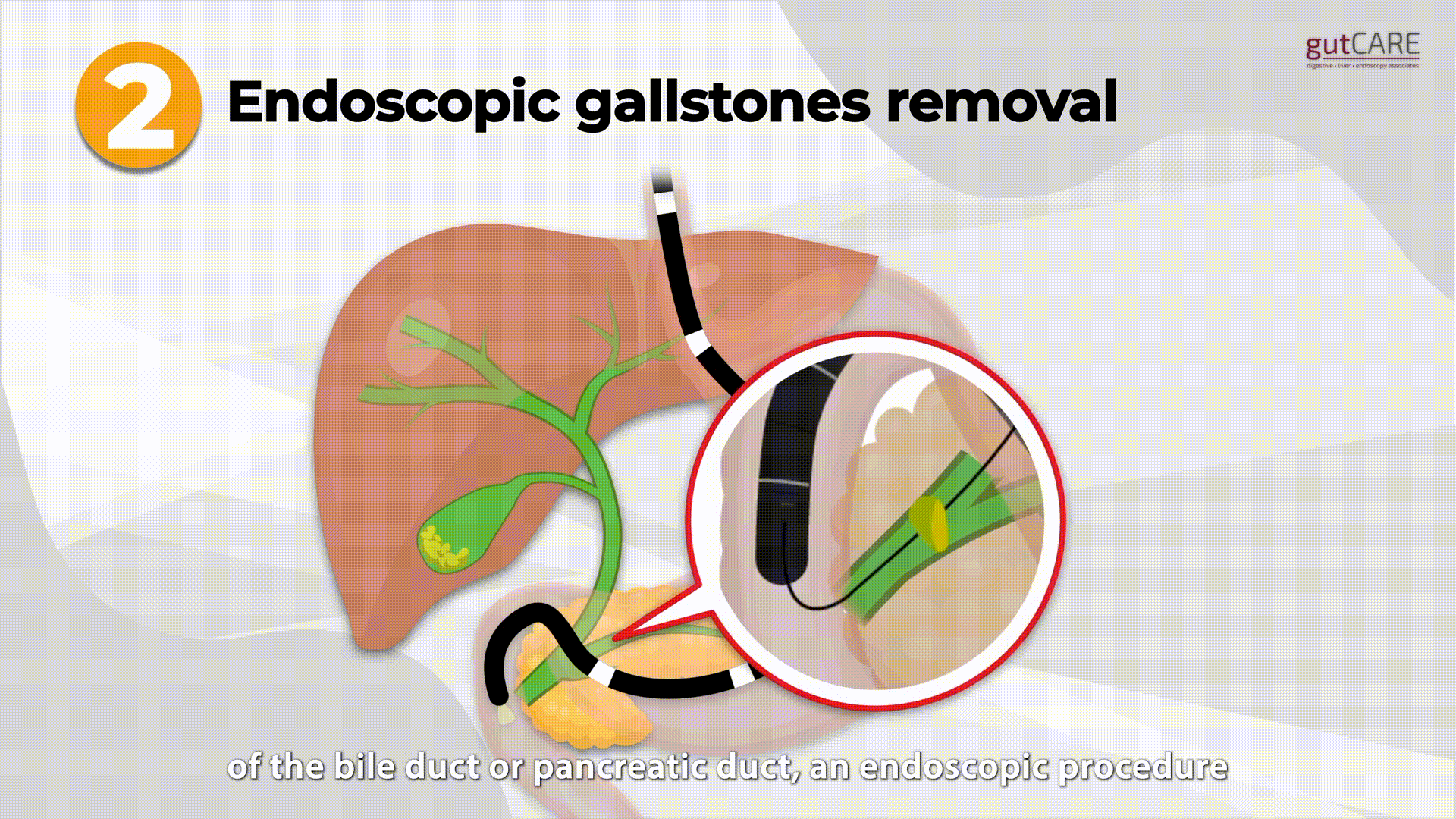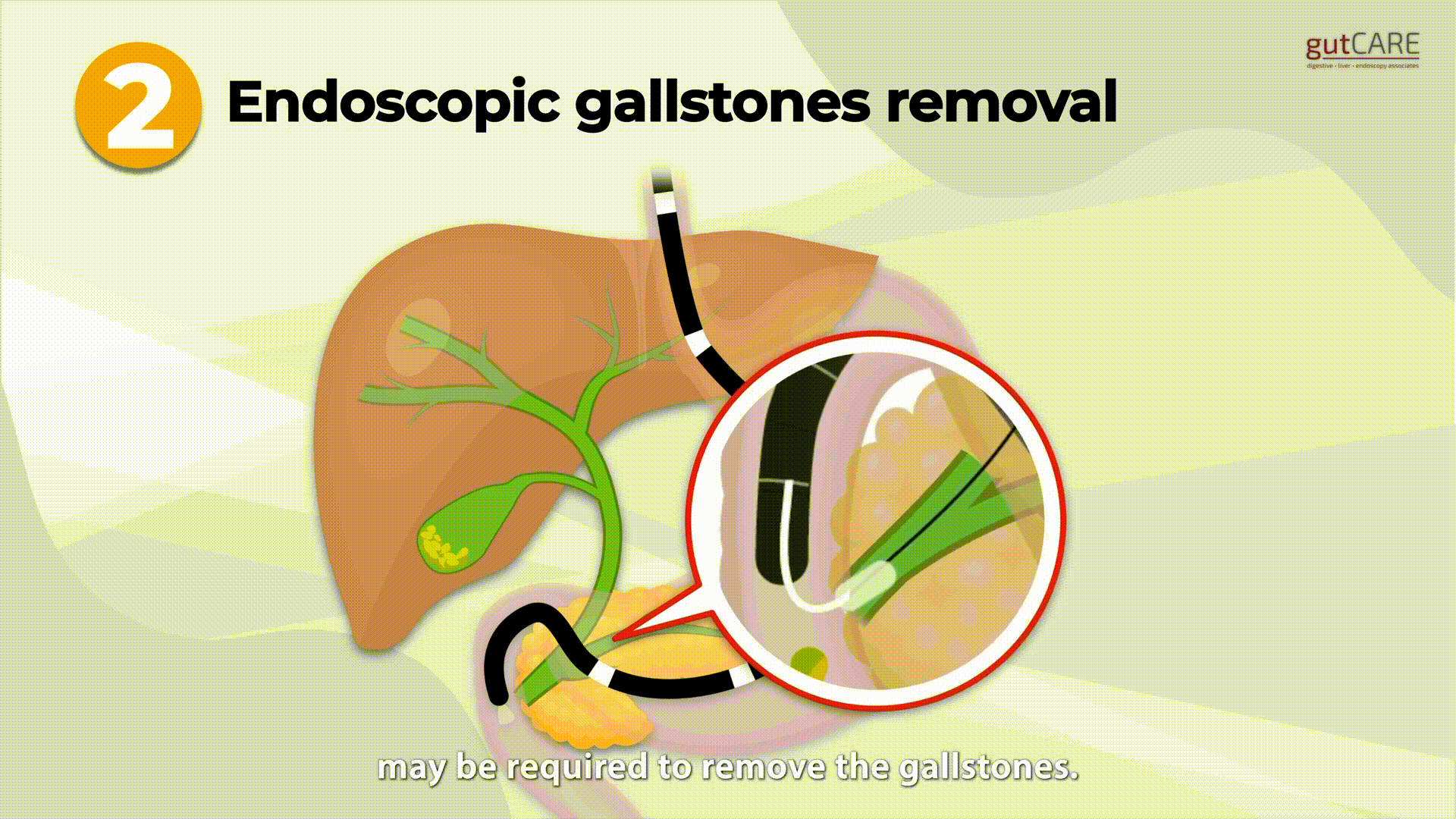
The endoscopist passes a special side viewing endoscope through the mouth into the duodenum to visualize the ampulla, which is the entrance to the bile and pancreatic ducts. Instruments are passed through the endoscope and guided through the ampulla and ducts using X-rays. These enable various treatments, including:
- Sphincterotomy: The muscle surrounding the opening is cut to enlarge it and facilitate various treatments.
- Stone removal: Stones may be removed from the ducts using baskets or balloons. Large stones may need to be crushed before removal.
- Stent placement: Stents are hollow tubes that are placed across blocked or narrowed areas in the duct to restore the drainage channel.
- Dilation: A special balloon is used to expand an area of the duct or its opening.
- Cholangioscopy: A special ultra-thin endoscope is passed into the bile duct to visualize the inside and enables precise tissue sampling or shattering of large stones.
INDICATIONS
ERCP can help to avoid surgery on the bile duct and pancreatic duct. ERCP is commonly used for:
- Removal of stones from the bile duct and pancreatic duct. This can relieve infection, jaundice, and pain and prevent future attacks.
- Insertion of stents to bypass narrowed and blocked areas. These are typically caused by tumours, stones, and scarring. This can relieve infection, jaundice and pain.
- Obtaining tissue samples from the bile duct to help make a diagnosis.
- Treat complications from the liver, bile duct or pancreatic surgery.
PREPARING For The Procedure
You should fast for at least 6 hours prior to your ERCP. You may drink clear fluid up to 2 hours before the procedure.
In general, most medications should be continued before an ERCP with the exception of diabetes medication and blood thinners. Diabetic medications should be omitted during the fasting period. You should check with your doctor if your blood thinners may be omitted before commencing the procedure.
BEFORE The Procedure
A nurse will conduct a final check and bring you into the procedure room. An intravenous line will be inserted. In some cases, medications such as antibiotics may be given before the ERCP. An anaesthetist will review and discuss with you the anaesthesia that will be given to keep you asleep and comfortable through the procedure.
DURING The Procedure
A throat spray will be administered to lessen the discomfort of the procedure. A plastic mouthpiece will be placed between your teeth to protect your teeth. You will be positioned lying on your belly. Both the endoscopic and radiologic equipment will be positioned accordingly. Sedation will be administered by the anaesthetist. After you have fallen asleep, the procedure will begin. You will likely not remember any parts of the procedure. You will be breathing on your own and monitored closely during the procedure. You will wake up gradually after the procedure is done.
AFTER The Procedure
You will be admitted overnight for observation. The nurses will give you food and drink once they assess that you have recovered from anaesthesia. They will continue to monitor you closely after the procedure and overnight so that any complications will be detected early. Sometimes, you may have a mild sore throat, bloating and cramping. This normally goes away after 24 hours.
If you are well, you will usually be discharged from the hospital in the following day unless there are other outstanding inpatient problems to be managed. Usually, an additional day of hospitalization leave is given for the following discharge. Your doctor will fix an appointment to explain the ERCP procedure and findings. He will then discuss the appropriate management plan.
SAFETY Of The Procedure
ERCP is a safe procedure relative to surgery for the same conditions. Major complications are rare and occur in less than 1% of cases. These are often due to disease factors. Such complications include tearing of the wall, bleeding and anaesthetic complications. Unfortunately, emergency surgery or intensive care may be required. Pancreatitis may occur in up to 5% of cases but can rise to 20-25% in certain populations. The overall risk is also higher in complex cases. Your doctor will advise you on the complications, what to watch for, and what to do should these occur.
QUALITY Of The Procedure
ERCP is an advanced endoscopic technique. The quality and safety of ERCP depend heavily on the specialist. Only a few endoscopists undergo additional years of training after specialization to perform ERCP properly. There are various levels of difficulty in ERCP. Most ERCP specialists are able to perform routine cases such as small stone removal or simple stenting. However, only experts are able to perform difficult cases successfully. It is important to ensure that the doctor performing the ERCP has the correct level of expertise to match the difficulty of the case.
COST Of The Procedure
An ERCP is a hospital procedure and is covered under most hospitalization plans. It is also Medisave deductible. Many companies’ health benefits and private health insurances cover the cost of a colonoscopy, which may extend to the private sector. The Ministry of Health provides fee benchmarks and publishes the average fees in each hospital. Before any endoscopic procedure, detailed financial counselling is done to help patients understand the cost breakdown. Patients should check with their insurance provider and do their own research before seeing a specialist.



